Uveitis/Ocular Inflammation
What is Uveitis?
Uveitis is inflammation of the uvea, the middle layer of the eye. The uvea is sandwiched between the sclera (the white part of the eye) and the nerve tissue (retina) inside of the eye (figure 1). The tissue has abundant blood vessels and usually has pigment. It is composed of three different parts, the iris, the ciliary body and the iris. There are many types of uveitis, some affecting the entire eye and some only affecting the front or back part of the eye. The inflammation from uveitis can cause damage to the eye that ultimately results in vision loss.
What causes Uveitis?
There are a lot of causes of uveitis. The severity and location of the inflammation can help guide the ophthalmologist as to what the underlying cause may be. However, in the majority of cases, the cause of the uveitis is never identified. Some of the more common causes of uveitis include autoimmune disease, eye injury and eye infections. These autoimmune diseases such as lupus or rheumatoid arthritis are conditions in which the body attacks its own tissue.
What are the symptoms of Uveitis?
Symptoms can range from very mild to severe. Common symptoms include eye redness, eye pain, sensitivity to light, floaters and blurry vision. The symptoms may occur suddenly or gradually develop and get worse with time. The symptoms may occur in one or both eyes.
How is Uveitis diagnosed?
Your ophthalmologist can detect uveitis through a careful and complete examination of the eye. Although the reason for the uveitis may never be identified, blood work is often done in order to identify any underlying body wide inflammatory disease or infections. A retinal scan called an Optical Coherence Tomography (OCT) is used to document if there is any damage or swelling to the retina at the back of the eye. A photographic test called a fluorescein angiogram may be done in order to tell the extent of damage to the uvea and related eye structures. This technique is also useful for evaluating possible underlying causes of uveitis.
What are the different types of Uveitis?
There are many different ways to classify uveitis. The most common and useful way is to classify the inflammation based on what structures in the eye have inflammation. Inflammation of only the iris or the front part of the eye is called iritis (figure 2). Inflammation of the back part of the eye or the choroid is called posterior uveitis (figure 3). If inflammation is located mainly in the middle of the eye near the ciliary body then it is called intermediate uveitis. All kinds of uveitis are potentially a very serious problem and should be treated promptly in order to decrease the risk of vision loss.
How is Uveitis treated?
Without treatment uveitis can cause severe permanent vision loss in many cases. If an underlying body-wide inflammatory disease or infection has been diagnosed, it is important to first make sure this is well treated. Often treating the underlying disease will help the eye. The main treatment for uveitis is anti-inflammatory medications. These medications are tailored to each case of uveitis. Sometimes simple anti-inflammatory eye drops can work, in other cases injections, oral medication or surgery may be needed to stabilize the disease. The inflammation from uveitis can cause damage to other structures inside of the eye. It is not uncommon to develop glaucoma (increased eye pressure), cataracts (whitening of the lens in the eye), or more severe complications from uveitis.
What is the long-term impact of Uveitis on my vision?
Most cases of uveitis respond to treatment. Treatment can slow down the disease and help prevent vision loss and the development of many of the associated complications. With prompt treatment, most patients continue to have good vision. For a small group of patients, medication alone is not enough to slow down the uveitis and surgery is needed to remove the vitreous gel from inside of the eye. The vision loss from uveitis can range from none in very mild cases to severe with almost complete loss of vision in more serious cases.
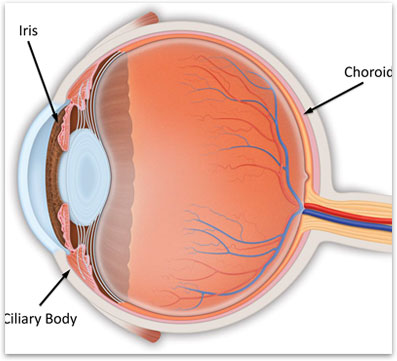
Figure 1. Anatomy of the eye showing the Uvea in relation to the rest of the eye.
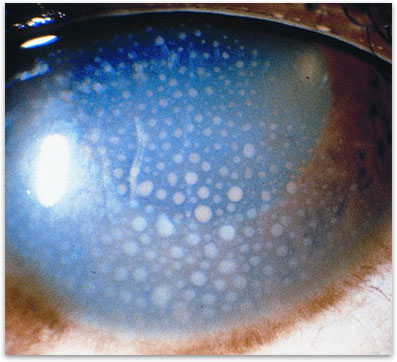
Figure 2. Iritis, note the whitish dots of inflammation on the inside of the cornea.
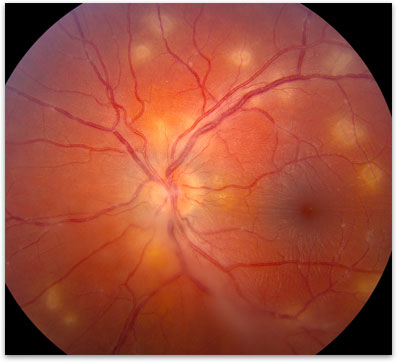
Figure 3. Posterior uveitis showing inflammation of the retina and the underlying choroid (white dots).

