Retinal Vein Occlusion
What is a Retinal Vein Occlusion?
The retina is a specialized layer of neural tissue that coats the back of the eye and is responsible for helping you to see. A retinal vein occlusion occurs when blood flow in one of the veins draining blood from the retina is reduced or blocked. Because blood that enters the eye cannot be drained properly through the blocked vein, the blood backs up in the retina creating areas of bleeding and swelling. The bleeding, swelling and lack of oxygen and nutrition in the retina can cause vision loss. Somewhat like a stroke occurring in the brain, in some cases the blockage in the vein can have very serious effects on the eye.
What causes a Retinal Vein Occlusion and who is at risk?
There are many different causes for a retinal vein occlusion. No single cause can explain the reason for every patient. The cause of a Retinal Vein Occlusion may be discovered thorough an evaluation of the retina or a general medical evaluation. Sometimes, the source of a Retinal Vein Occlusion cannot be identified, despite having a through examination and testing. Typically this condition occurs in individuals greater than 50 years old. Diseases that can contribute to the formation of a Retinal Vein Occlusion include high blood pressure, diabetes, heart disease, blood clotting disorders and glaucoma. The other eye can develop a retinal vein occlusion in 10% of people.
Are there different types of Retinal Vein Occlusions?
There are two major categories of retinal vein occlusions, branch and central retinal vein occlusions. The veinous drainage system for removing blood from the eye can be likened to a tree with many small branches draining into larger ones and ultimately into one central retinal vein (the tree trunk). In a branch retinal vein occlusion (BRVO) a small branch of the retinal venous system becomes blocked (figure 1). In a central retinal vein occlusion (CRVO) the primary trunk of this vein can become blocked (figure 2).
What are the symptoms of a Retinal Vein Occlusion?
Retinal vein occlusions encompass a spectrum of disease ranging from mild, having little or no impact on the vision to severe, leading to blindness in the eye. The symptoms depend on the size and precise location of the blockage. Most patients note a sudden blurring or distortion of the vision that can be associated with a blind spot. The vision loss is usually not associated with any pain.
How is a Retinal Vein Occlusion diagnosed?
Your retina specialist can diagnose a vein occlusion by examining your eye and using specialized testing to confirm the diagnosis. A photographic dye test called a fluorescein angiogram can be used to identify the location of blockage and the extent of the loss of blood flow. Optical coherence tomography (OCT) is used to obtain a high-resolution anatomic scan of the retinal structure (figure 3). This technique is useful in documenting the degree of swelling in the retina and monitoring response to treatment (figure 4).
What are the complications of Retinal Vein Occlusions?
Macular Edema
After a vein occlusion the small retinal blood vessels near the center of your eye can start to leak. If the eye develops a lot of leakage the retina can become swollen and your vision can become worse. This is called macular edema.
Neovascularization
In severe cases of retinal vein occlusion where the retina does not get enough oxygen abnormal blood vessels can grow inside the eye (neovascularization). These new blood vessels are very problematic because they tend to bleed. In severe cases bleeding can occur in the vitreous cavity or severe glaucoma can develop from the blood vessels growing near the front of the eye. Left untreated, these changes can result in irreversible blindness.
How is a Retinal Vein Occlusion treated?
Good control of your diabetes, high blood pressure, or glaucoma, if present, is very important in caring for your eye and preventing further damage to your vision. There is no known cure for retinal vein occlusion. The focus of treatment is to treat the complications of retinal vein occlusions, macular edema and neovascularization. Both macular edema and neovascularization are treated with intraocular injections, laser surgery, or rarely surgery.
What is the prognosis?
The prognosis depends on the extent of damage from the vein occlusion. Fortunately, many patients can expect to regain good vision. Some will have poor vision due to loss of blood supply or retinal damage from chronic swelling in the macula. Your retina specialist can talk with you more about your individual prognosis.
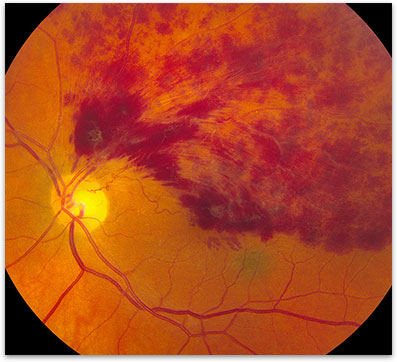
Figure 1. Branch Retinal Vein Occlusion
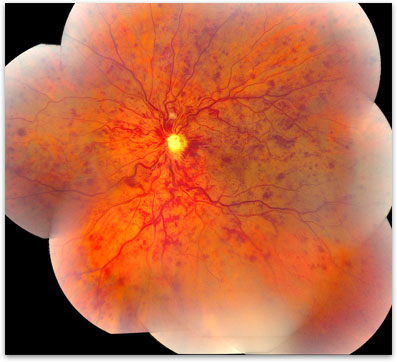
Figure 2. Central Retinal Vein Occlusion
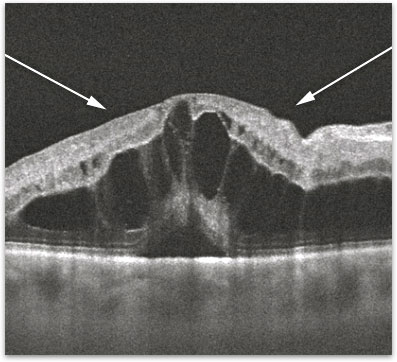
Figure 3. OCT of Vein Occlusion associated macular edema.
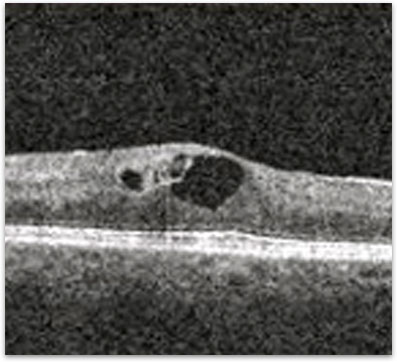
Figure 4. OCT showing the resolution of the edema in the retina in response to Anti-VEGF therapy.

