Ischemic Optic Neuropathy
What is Ischemic Optic Neuropathy?
The optic nerve is the central nerve that carries sight from the eye to the brain. It is composed of over 1 million neurons. Damage to the optic nerve is called optic neuropathy. Ischemic optic neuropathy (ION) is a sudden loss of central vision and/or side vision because of poor blood flow to the optic nerve (figure 1). There are two main forms of ION, arteritic (aka Temporal arteritis) and nonarteritic (aka NAION)
What Causes Ischemic Optic Neuropathy and who is at risk?
NAION- The exact reason for the reduced blood flow in NAION is unknown. NAION is the most common type of ischemic optic neuropathy and usually occurs in individuals over 40. Most people who develop NION have underlying high blood pressure, diabetes, sleep apnea or high cholesterol. Smoking may increase the risk of developing NAION. Rarely some medications have been known to cause NAION.
Temporal Arteritis
A less common type of ION occurring in people over 50 years of age. This disease is an inflammatory disease that affects certain medium to large-sized blood vessels, including those in the eye. The exact cause of the inflammation is unknown, but the inflammation of the blood vessels cause a loss of blood flow to the optic nerve (figure 2).
What are the Symptoms of Ischemic Optic Neuropathy?
Sudden loss of central or side vision is the most common symptom. You may notice loss of side vision in the lower half of reading vision. ION generally does not cause any other symptoms, such as pain or double vision. The risk of brain stroke is no greater for people with ION. People with temporal arteritis often have many more symptoms. Headaches, and tenderness over the temple region is common. Joint aches and pains commonly affect the shoulders and hips. They may also feel tired and run a fever, combined with recent weight loss.
How is Ischemic Optic Neuropathy diagnosed?
Your ophthalmologist will perform a complete eye examination, including pupil dilation. Decreased blood flow usually results in swelling of the optic nerve, which your ophthalmologist can see when he or she looks into your eye. A test of side vision (visual field), may also be performed. In addition, a blood test and/or biopsy of an artery in the temple to diagnose temporal arteritis may be required.
How is Ischemic Optic Neuropathy treated?
NAION- there is no proven treatment for NAION. Involvement of the other eye occurs in about 20-30% of people. Therefore it is very important to work with your primary care physician to make sure any underlying diabetes, high blood pressure, high cholesterol or sleep apnea is under control. Some researchers believe that taking blood pressure medications at night can contribute to NAION. If possible try and take any blood pressure medications in the morning.
Temporal arteritis
Patients with temporal arteritis have a very high chance of losing vision in the other eye unless treatment is started. Treatment involves using steroids at a high dose. The anti-inflammatory effects of the steroids decrease the risk of losing vision in the other eye.
What is the long-term impact of Ischemic Optic Neuropathy on my vision?
NAION- In some cases the vision can get worse over the first few weeks. Vision in the affected eye will typically stabilize within two months. Unfortunately in most cases some vision loss is permanent. Approximately 40% of eyes with moderate vision loss can have at least some improvement in the vision over the first few months.
Temporal Arteritis
Typically vision loss is usually very severe and usually does not improve very much with treatment. In general, the vision usually stabilizes once steroids are started. Some people can have a small degree of vision improvement with steroids. For those with severe vision loss in both eyes, often some side vision is preserved. This side vision generally allows you enough sight to function at home independently. Special visual devices are available which can help you to continue many daily activities.
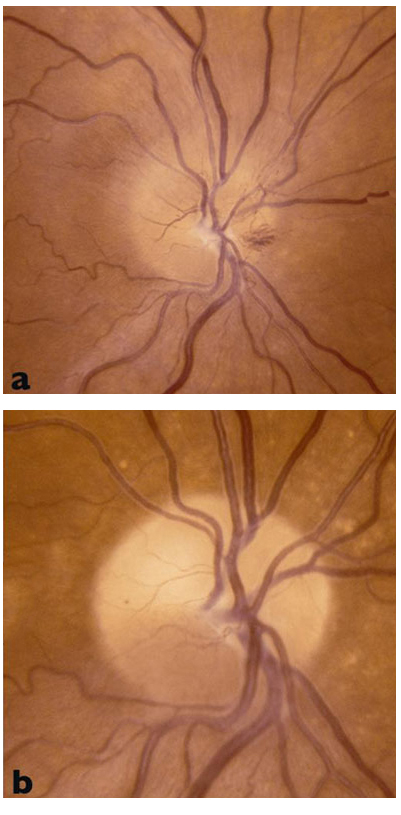
Figure 1. Optic nerve with a loss of blood flow from NAION, (a) shows the appearance of the optic nerve right after the damage, (b) shows the optic nerve months later. Note the yellowing or pallor of the optic nerve in image (b).
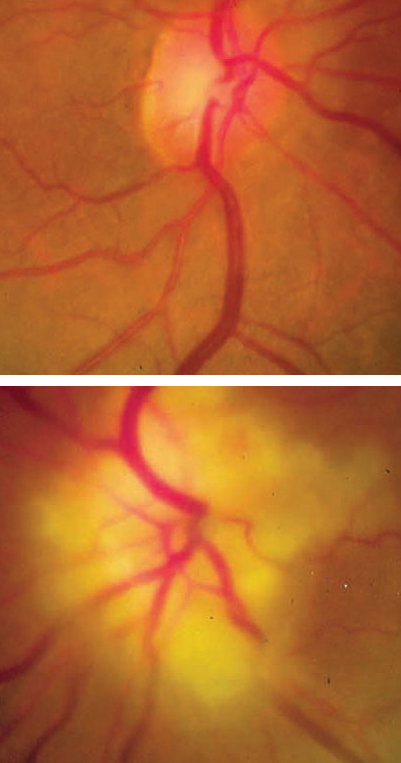
Figure 2. Optic nerves of a patient with temporal arteritis. Top image is of normal right eye, Bottom image shows swollen optic nerve in the Left eye.

